It has come to my attention that many of my patients have been told they have arthritis, but don’t know which kind or what really causes it. First off, there are many different kinds of arthritides (plural for arthritis). There are metabolic arthritides such as gout where too much uric acid builds up in the joints and forms crystals that damage the joints; there are autoimmune diseases like rheumatoid arthritis that tricks the body into attacking the connective tissue in joints; there is the possibility of an infection in the joint that leads to arthritis; but the most common type of arthritis is osteoarthritis, and this is usually what a doctor means when he/she tells you that you have arthritis.
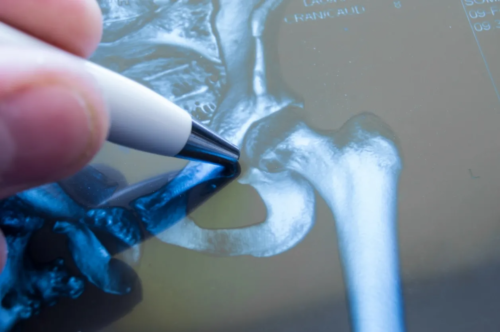
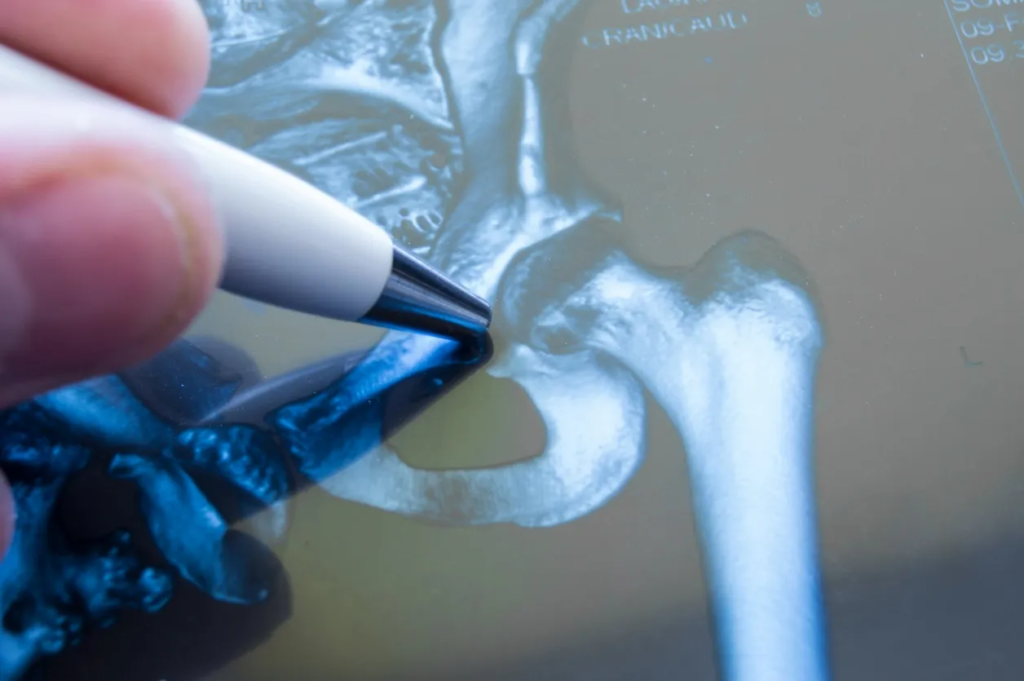
So, what is osteoarthritis? This type of arthritis is known by many names: spondylosis, degenerative joint disease, degenerative arthritis, degenerative arthrosis, arthrosis, and several more uncommon terms. Osteoarthritis (OA) is nicknamed the wear-and-tear disease of the joints. This is because OA is the result of excessive stress in the form of tension, friction, and compression that repetitively occur over time causing degeneration of the elements of the joint that keep it moving smoothly. This degeneration leads to stiffness, pain, swelling, and those grinding/clicking/popping noises called “crepitus”. Osteoarthritis is often found along side other types of problems related to excess physical stress like degenerative disc disease, herniated discs, tendinitis, and bursitis. Each joint in the body is susceptible to OA, but as you can imagine it shows up more often in joints that bear more weight and stress like hips and knees. Typically a doctor will diagnose you with OA by X-ray. Changes we look for are: loss of joint space (which indicates erosion and damage to the cartilage), pieces of bone loose in the joint, bone spurs, enlargement or thickening of the bone around the joint, alteration of the alignment of the joint, deformity of the joint, and a handful of other findings. Doctors may use the term “bone-on-bone” when it gets bad enough that there is no more cartilage.
The most important thing to remember here is that osteoarthritis is the result of excessive wear and tear from bad joint mechanics. Many of my patients will say something like “Well Doc, I’m just getting old”. My reply is usually to ask if one of their knees is older than the other. Because, if OA is truly due to age, then why does one side typically start to have problems before the other? It is true that the older a body is, the more opportunities it has had to undergo wear and tear, and the more likely that damage will result in OA. But, time and old age by itself does not produce OA. The alteration of the mechanics of the joint results in OA. There has to be a problem with the joint, and this problem leads to damage over time that finally culminates in this type of arthritis.
Attributing arthritis to old age is associated with falsely accepting that there is nothing that can be done about the problem. Nothing could be further from the truth. It may be true that the more advanced the OA, the harder it can be to treat, but this does not mean that the problem should be ignored. In the medical world, this mind-set is called “taking on the sick role”. Don’t take on the sick role! If you decide to do nothing about the problem, it will continue to get worse. It is much better to nip OA in the bud rather than let it get so bad that the only realistic solution includes joint replacement surgery. Once you have that surgery, things will never be the same. The biomechanics in the area will permanently be altered, not to mention the risks of surgery or the recovery/rehab or the expense. The point is, don’t let it get to the point of surgery. That old trick knee or a past accident/injury can be the beginning of OA, but it doesn’t have to end in full blown OA. Even if the osteoarthritis is advanced, and even if a surgery needs to be performed, the underlying dysfunction that caused the arthritis is still there and needs to be corrected, or problems will continue/reoccur. So, you are going to have to address this no matter which way you go. Better to correct it sooner than later.
I want everybody to understand something. Every joint in the body is meant to be in a certain position and move a certain way. As the two joint surfaces move relative to one another, they are meant to remain congruent, or flush against each other. Imagine a ball and socket joint. If the ball is not centered in the middle of the joint as it goes through it’s motions, then the ball rides up on one side of the cup grinding and causing excessive friction. This damages the joint and leads to further changes. Alterations in the balance of the muscles and/or ligaments around the joint result in bad joint mechanics. This can be from an injury or a bad habit like improper posture. Muscles are important because they keep that joint centered in the correct position as the joint goes through it’s movement. If the muscles are not balanced, then the joint capsule becomes stretched and altered. These joint capsules are made up of ligaments that connect one bone to another. It is composed of fibrous material that ensures that the bones are held together tightly and keep the bone from sliding too far in any direction. If you have ever heard of an ACL tear, then you know that this important ligament keeps the knee from shifting forward, and if damaged, the knee becomes unstable because there is nothing to keep the motion in check. These ligaments/joint capsules can actually become stretched and warped with repetitive damage. The capsule will be tight and shortened on one side and stretched long on the other. If this happens, they no longer do their job and the joint rides out of place. If left uncorrected, these types of abnormal joint mechanics will lead to OA.
Now that you understand how these alterations can lead to damage ultimately resulting in OA, you probably want to ask…How do we fix this? Well, it’s not easy–you are going to need an expert (and I’m not talking about a personal trainer). It all comes down to re-balancing the joint: this includes the muscles and the ligaments. The first thing we need to do is get the tension of that joint capsule equal again. We need to stretch the shortened side. This is the side(s) where there is a restriction in the range of motion (ROM). This can be done with manipulation or adjustment. The next thing we need to do is stretch the tightened muscles. This can be done by a health care provider or by the patient themselves; preferably a combination of the two. This takes time, but once the ROM has been normalized, it is time to strengthen the correct set of muscles around the joint. If you try to strengthen the muscles first without normalizing the ROM, it is possible that you will be doing more damage by reinforcing the bad pattern. It would be like running after you sprain an ankle. Once those muscles are correctly stretched and strengthened in the right pattern, this will keep the joint centered and eventually the capsule will heal and normalize again because the capsule/ligament fibers shrink up over time if they are not always being stretched out. So if the muscle does its job keeping the ROM of the joint in check, then the ligament/capsule has an opportunity shorten back up to it’s normal length thereby re-establishing it’s ability to correctly stabilize the joint.
This process takes time. Treatment should be approached as a coordinated effort between the physician and the patient working as a team. Furthermore, both physician and patient should be patient, expecting progress to happen slowly over time: especially if the problem has existed for a long time. It is also important to understand that pain is not a good indicator of when the problem has been fixed, but rather by the ROM and balance in the joint. This is because it typically takes quite a bit of dysfunction and damage to start producing painful symptoms. So when treatment alleviates the pain, this is usually only about 20% progress. The joint is still dysfunctional and if the joint does not get properly balanced and stabilized, then the condition will return. At this point, the patient will have lost a lot of progress. Don’t throw away your time and money: finish the treatment just the way you would finish out your antibiotic even if you are feeling better.
If you have arthritis, or a painful or stiff joint that isn’t getting better, or if you have had a recent injury, then please seek out a Chiropractic Physician. This is our bread and butter. A Chiropractor treats OA like a dentist treats tooth decay: it is our main work. If you have any questions, please contact our clinic.